Osteoarthritis In Dogs And Cats
3/28/20267 min read
WHEN EVERY STEP HURTS: UNDERSTANDING OSTEOARTHRITIS IN YOUR DOG OR CAT
One of the most common — and most overlooked — conditions affecting our aging companions, explained for the people who love them most.
Your dog used to bound up the stairs without a second thought. Your cat used to leap onto the windowsill as though gravity was optional. Now there's a hesitation — a wince, a slow creep, a reluctance that wasn't there before. Osteoarthritis might be why.
Osteoarthritis (OA), also called degenerative joint disease, is the single most common musculoskeletal condition in both dogs and cats. It affects an estimated 20% of adult dogs and possibly 40% or more of cats over the age of ten — numbers that should make every pet owner pay attention. Yet because animals are wired to hide pain (a survival instinct inherited from their wild ancestors), OA often progresses quietly for months or years before anyone notices.
The good news: once you know what to look for, there's a great deal you and your veterinarian can do together to improve your pet's comfort and quality of life.
WHAT EXACTLY IS OSTEOARTHRITIS?
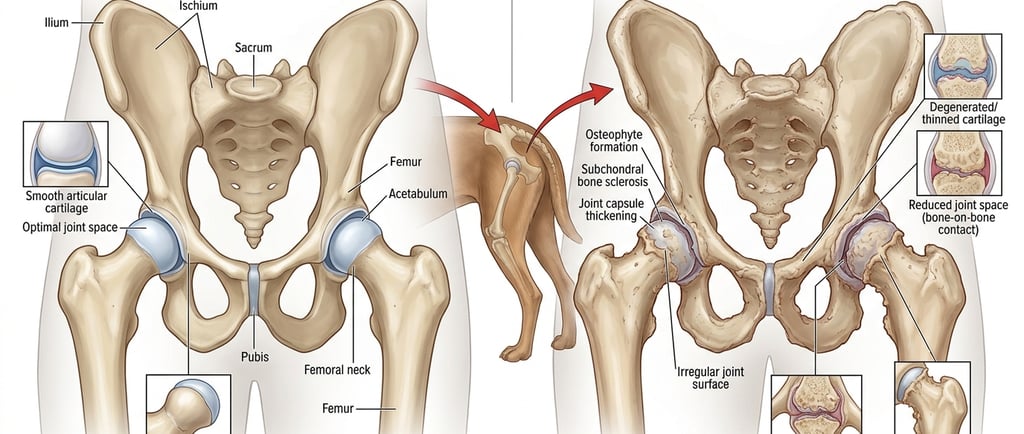
Healthy joints are cushioned by a layer of smooth, slick cartilage that allows bones to glide past each other almost frictionlessly. Synovial fluid — a thick liquid produced by the joint lining — acts as a lubricant and shock absorber on top of that.
In osteoarthritis, that cartilage begins to break down. The process is gradual but relentless: the surface becomes rough and pitted, the synovial fluid loses its protective properties, and the underlying bone starts to change shape in response to the abnormal stress. The joint lining becomes inflamed. Bone spurs (osteophytes) can form. Eventually, in severe cases, bone may rub against bone.
This is a progressive, chronic condition — meaning it cannot be reversed, but it absolutely can be managed. The goal of treatment is not a cure but a return to comfort.
Did you know: OA is not just a disease of old age, though aging is the biggest risk factor. Large and giant breed dogs are disproportionately affected, and pets with prior joint injuries, hip or elbow dysplasia, or a history of obesity are at significantly higher risk — sometimes developing OA as young adults.
SPOTTING THE SIGNS: DOGS VS. CATS
This is where it gets tricky. Dogs and cats express pain very differently, and cats in particular are so good at concealing discomfort that even attentive owners are often blindsided by the diagnosis.
In dogs, watch for:
Stiffness after rest, especially in the morning
Reluctance to climb stairs or jump into the car
Visible lameness or "bunny-hopping" gait
Swollen or warm joints
Licking, chewing, or guarding a joint
Reduced enthusiasm for walks or play
Muscle wasting in the affected limb
Irritability when touched or petted
In cats, watch for:
Jumping less high, or refusing to jump at all
Difficulty using — or eliminating outside — the litter box
Reduced grooming or unkempt, matted coat
Increased hiding or withdrawal
Over-grooming or hair loss above a joint
Changes in sleep location (lower surfaces)
Decreased appetite or activity
Unusual aggression when handled
Important: Cats rarely limp overtly from OA. A limping cat is relatively uncommon — but a cat in significant arthritic pain is not. Behavioral and lifestyle changes are often the only clues. If your cat seems "just getting old," bring it up with your vet; that phrase describes many arthritic cats.
GETTING A DIAGNOSIS
There is no single blood test for OA. Diagnosis is based on a combination of a thorough physical examination (including manipulation of each joint to assess range of motion, pain response, and swelling), your observations at home, and X-rays (radiographs). X-rays can show joint space narrowing, bone spurs, and other characteristic changes — but it's worth knowing that the severity visible on X-ray doesn't always match the severity of pain. A pet with mild radiographic changes can be in significant discomfort, and vice versa.
For cats especially, your vet may ask detailed questions about behavior at home — videos you've taken of your cat's movements and daily routine can be incredibly helpful. Some clinics use validated pain-scoring questionnaires designed specifically for cats and dogs with chronic pain.
TREATMENT: BUILDING A MANAGEMENT PLAN
OA management is not a single pill — it's a layered, individualized approach that combines medication, physical support, weight management, and lifestyle adjustments. The most effective plans are built collaboratively with your veterinarian and adapted as your pet's needs change over time.
Medications your vet may discuss with you:
NSAIDs (Non-steroidal anti-inflammatory drugs): The most commonly prescribed class for OA pain in dogs. Veterinary-specific NSAIDs like carprofen, meloxicam, grapiprant, deracoxib and others reduce joint inflammation and pain effectively. They require regular blood monitoring and should never be combined. NSAIDS and corticosteroids (e.g. prednisolone) should never be used together as significant stomach upset can happen. Cats can use meloxicam but require very careful dosing; feline NSAID options are more limited than for dogs.
Monoclonal antibody therapies: A newer class — nerve growth factor (NGF) inhibitors given by injection once monthly. Librela (bedinvetmab) is licensed for dogs and Solensia (frunevetmab) for cats. These target a specific pain-signaling pathway and are proving very effective, particularly for cats where NSAID options are more restricted.
Joint supplements: Omega-3 fatty acids (particularly EPA and DHA from fish oil) have the best evidence base for reducing joint inflammation. Glucosamine and chondroitin are widely used and generally safe; evidence is mixed but some pets respond well. These are adjuncts, not replacements for prescription therapy.
Gabapentin / amantadine: Used for nerve pain and "wind-up" — the process by which the nervous system becomes sensitized to pain signals over time. Often added to multi-modal plans for pets with moderate to severe OA, or those who don't fully respond to NSAIDs alone.
Polysulfated glycosaminoglycan injections (Adequan): Given as a series of injections, this compound is thought to help protect and support remaining cartilage. Commonly used as part of early management protocols, particularly in dogs.
⚠ Never give these to your pet: ibuprofen (Advil/Nurofen), naproxen (Aleve), acetaminophen/paracetamol, or any human NSAID. Human pain medications are frequently toxic — sometimes fatally so — to both dogs and cats. Always consult your vet before giving anything over-the-counter.
Physical therapies worth asking about:
Veterinary physiotherapy (also called rehabilitation therapy) is an expanding field with real benefits for arthritic pets. Hydrotherapy (swimming or underwater treadmill) is particularly valuable — the buoyancy of water allows joints to move without bearing full body weight, building muscle and improving mobility without pain. Laser therapy, acupuncture, and massage are used at many clinics and can complement medication well.
THE WEIGHT CONVERSATION
This one matters enormously. Excess body weight is one of the most significant modifiable risk factors for OA severity. Every extra kilogram places dramatically increased mechanical stress on joints — particularly hips, knees, and elbows. Studies in dogs have shown that lean body condition can delay the onset of OA in dogs predisposed to hip dysplasia by years, and substantially reduce pain scores in dogs already diagnosed.
Many vets estimate that between 40–60% of pet dogs in the UK and US are overweight or obese. If your vet mentions weight, it isn't a judgment — it's one of the most genuinely helpful interventions available, and it works.
Practical tip: You should be able to feel (not see) your pet's ribs with light finger pressure, with a thin layer of fat over them. If you have to press firmly to feel ribs, or can't feel them at all, that's a signal to discuss weight management with your vet. Your vet may give your pet a Body Condition Score: this is a value between 1 and 9 with 1 being very emaciated and 9 being very obese; 4-5 is ideal. Clinical studies have shown that pets in their ideal weight range live an average of two years longer!
MAKING HOME A MORE COMFORTABLE PLACE
Simple environmental modifications can make a surprising difference to daily comfort:
Thick, supportive orthopedic bedding placed at floor level
Pet ramps or steps to sofas, beds, and favorite spots
Non-slip mats on hard flooring (tiles, wood, laminate)
Shorter, more frequent walks for dogs rather than long ones
Low-sided litter tray for cats with hip or spinal OA
Raised food and water bowls for dogs with neck or shoulder pain
For cats, think vertically: rearranging furniture so they can access their preferred heights by stepping rather than jumping can preserve independence and reduce frustration. Keeping warm is also helpful — many arthritic pets are more comfortable in mild temperatures and may gravitate toward warm spots instinctively.
EXERCISE: LESS IS NOT ALWAYS MORE
A common misconception is that rest is best for an arthritic pet. In reality, appropriate, low-impact exercise is one of the best things for arthritic joints. Movement maintains muscle mass (which supports and stabilizes joints), prevents stiffness, and supports a healthy weight. "Appropriate" is the key word: the aim is gentle, consistent activity rather than sporadic bursts.
For dogs, this means regular short walks at a comfortable pace — the same route at the same time each day is often better than varying distances. Swimming, if your dog tolerates it, is excellent. Avoid high-impact activities like jumping, sharp turns, and chasing balls, especially on hard surfaces.
For cats, encourage gentle play with low-effort toys (a dragging feather wand moved slowly across the floor rather than overhead leaping games). Puzzle feeders that don't require acrobatics can keep minds sharp and bodies gently moving.
A pet that moves more comfortably after light activity has warmed up is typical of OA. The "morning stiffness" pattern — worse at rest, better after gentle movement — is classic. This is not a sign that exercise is harmful; it's a sign the management plan is on the right track.
MONITORING AND FOLLOW-UP
OA is a lifelong condition, and treatment needs will change over time. Most vets recommend check-ups every three to six months for pets on ongoing medication — both to assess pain control and to monitor for any side effects. Blood tests are typically recommended every six to twelve months for pets on NSAIDs.
Between visits, keeping a simple daily journal — or even short phone videos of your pet walking and navigating the home — gives your vet invaluable information. Pain scoring tools designed for home use, like the Helsinki Chronic Pain Index for dogs or the Feline Musculoskeletal Pain Index for cats, can help you track changes objectively.
If your pet seems less comfortable despite their current treatment, it's always worth going back to your vet rather than waiting. Multi-modal pain management — combining two or more complementary approaches — is often far more effective than any single treatment, and there may be options you haven't tried yet.
A FINAL WORD
Caring for a pet with osteoarthritis asks something of us: to pay closer attention, to notice the quiet signals, to become advocates for a companion who cannot tell us where it hurts. It also offers something: the knowledge that with good veterinary care and an attentive home environment, arthritic pets can live genuinely comfortable, happy lives for years after diagnosis.
The first step is always the same — a conversation with your vet. If anything in this article has made you wonder about your own dog or cat, that conversation is worth having.
This article is for educational purposes only. Always consult a licensed veterinarian for diagnosis and treatment decisions. Content does not replace professional veterinary advice, diagnosis, or treatment.
© 2026 vetcareinco.io
Contact
The information provided on this website is intended for general informational and educational purposes only and does not constitute veterinary medical advice. It is essential to consult with a qualified veterinary professional for any health concerns or before making any decisions related to your pet's health or treatment. We are not liable for any actions taken or not taken based on the information provided on this website.
DrRobert@vetcareinfo.io
© 2025. All rights reserved.
